
Implants • 3D scans • Birmingham & Walsall
Looking for Dental Implants in Birmingham or Walsall?
Natural-looking, long-lasting tooth replacement with a clear plan from day one. We offer free implant consultations, 3D scanning where needed, and tailored treatment plans — from single implants to full-arch solutions.
Clear options. No rushing. No pressure. Comfort and patient control come first — and we only proceed when you’re comfortable.
Not sure which option is right? Start here: Replacing missing teeth — your options.
Great Barr clinic: 341 Birmingham Road, Great Barr, Birmingham, B43 7AP

Calm, honest care — led by the same dentist throughout
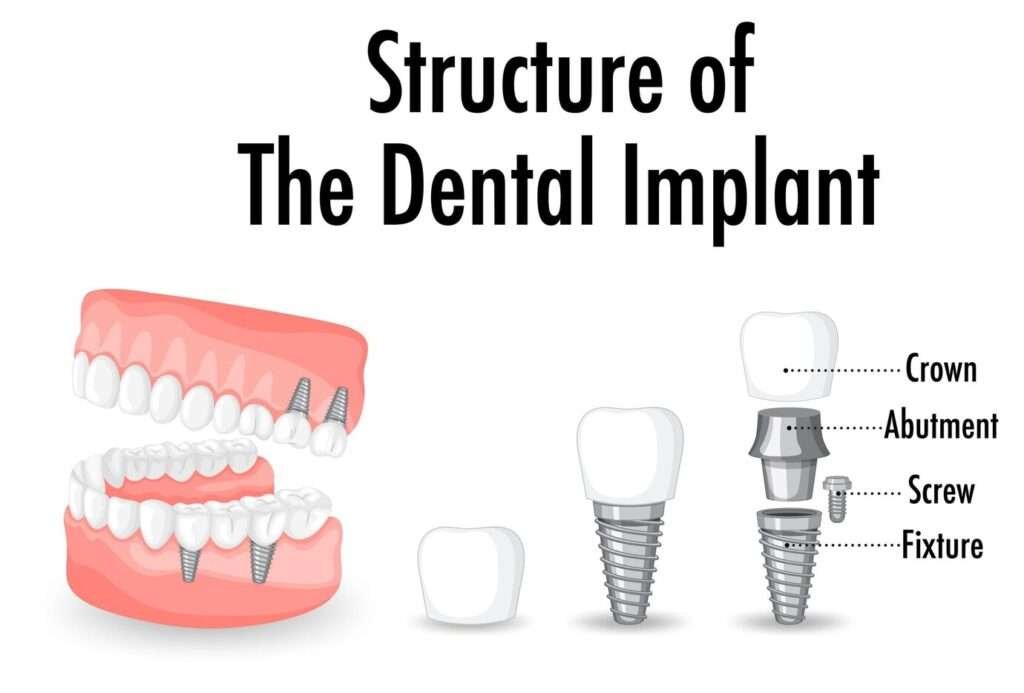
What an implant actually is
A small titanium post supports a crown, bridge, or denture — giving you a stable bite and a natural look.
If a scan is needed for safe planning, 3D scans start from £139 per arch per arch.

Why choose us for dental implants?
No obligation. No pressure to proceed after your first visit. We take time to plan properly and explain your options clearly.
Same dentist, start to finish
You’re guided by the same clinician through planning, treatment, and aftercare.
Honest advice, never pressure
If implants aren’t right for your case, we’ll explain practical alternatives.
Comfort & control first
We don’t rush or push through pain. We pause, adjust, or stop — and only continue when you’re comfortable.
Fast, responsive appointments
Clear next steps and sensible timeframes, with help if anything changes.
Helpful reads: What are dental implants? • How to clean implants • Why implants fail • Loose implant crown repair

Dr Rikki Dhody
Implant care should feel straightforward: clear options, careful planning, and a predictable route forward — with honest alternatives if implants aren’t right for your case.
- Planning-led approach: X-rays and 3D scanning where needed to plan safely.
- Clear explanations: what’s realistic for your bite, bone levels and gum health.
- Long-term focus: maintenance, cleaning access, and aftercare so results last.
Based in Great Barr, supporting patients across Birmingham, Walsall, West Bromwich, and Sutton Coldfield.
Why choose private dental implants?
Long-lasting
With good care, implants can last for many years and often decades.
Natural look & feel
Your crown is made to match your teeth for a seamless result.
Stable bite
Eat and speak with confidence — no adhesives, no slipping.
Helps preserve bone
Implants support the jaw, helping reduce long-term bone loss.
If you’ve been looking for private implants with personalised attention and minimal waiting, our Great Barr clinic supports patients across Birmingham and Walsall.
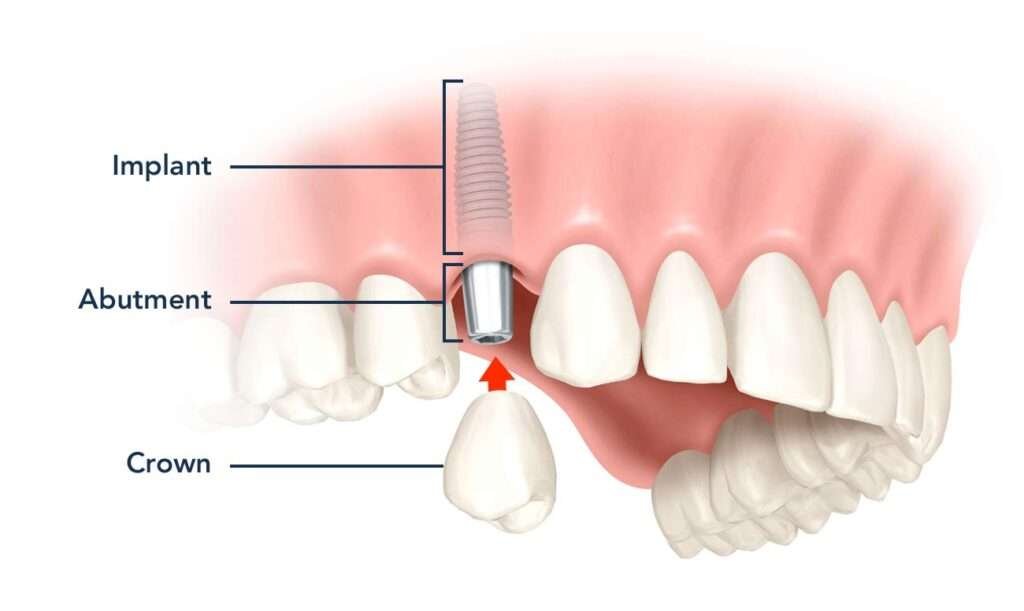
Single tooth implants
A single implant and crown can replace a missing tooth without preparing neighbouring teeth (unlike a bridge).
Typical range: £2,100 – £3,360 (case-dependent). Learn more: Single tooth implants.
Multiple teeth
Implant bridges can replace several missing teeth with fewer implants — often a strong balance of function and cost.
We’ll advise what’s realistic for your bite, bone levels, and hygiene.
Useful comparison: Dentures vs implants.
Full-arch options (including All-on-4)
If you’re missing most or all teeth, full-arch implant solutions can give a fixed, stable result. We’ll confirm whether you’re suitable, whether grafting is needed, and what timeline makes sense.
- All-on-4 style plans (where appropriate)
- Fixed bridge options
- Implant-supported dentures for added stability
Typical range: From £18,375 – £26,250 per jaw. Learn more: All-on-4 implants.
Step-by-step implant process
- Consultation: goals, assessment, and scans/X-rays as needed (implant consults are free).
- Planning: a clear plan (and alternatives if implants aren’t right).
- Placement: implant placed carefully under local anaesthetic (sedation options where appropriate).
- Healing: the implant integrates with the bone over time.
- Final teeth: crown/bridge/denture fitted for function and aesthetics.
We’ll guide you on aftercare and long-term maintenance so your implant stays healthy. If you want to prepare, read: How to clean dental implants.
How much do dental implants cost?
Costs depend on the number of teeth, bone levels, gum health, and the type of final teeth (crown/bridge/denture).
- Single implant (typical range): £2,100 – £3,360
- All-on-4 / full arch (typical range): From £18,375 – £26,250 per jaw
- 3D scans (if needed): from £139 per arch per arch
For a deeper breakdown: Implant costs explained • Full price list

Patient success stories
Real patient words — short clips, straight to the point.

Dental implant FAQs
Are implants painful?
Most patients describe pressure rather than pain during treatment. We use effective local anaesthetic, work gently, and you stay in control throughout.
How long does the implant process take?
It depends on healing and whether additional steps are needed. We’ll map out a clear timeline after your assessment (and any scans, if required).
Do I always need a 3D scan?
Not always. If we need extra detail for safe planning, 3D scans start from £139 per arch per arch.
How much does a single implant cost?
Typical range is £2,100 – £3,360 (case-dependent). A free implant consultation helps confirm the best plan for you.
How much does All-on-4 cost?
Typical range is From £18,375 – £26,250 per jaw. We’ll confirm suitability and the most sensible long-term option.
What if I’ve been told I don’t have enough bone?
Some cases need grafting or an alternative plan. We’ll assess your bone levels and explain options clearly before you decide.
Can implants fail?
They can, usually due to infection, biting overload, or cleaning challenges — but good planning and aftercare reduces risk. Read: Why implants fail.
My implant crown feels loose — what should I do?
Avoid chewing on it, don’t try to glue it, and book an assessment so we can confirm what’s loose (crown/abutment vs implant) and secure it safely. See: Loose dental implant crown repair.
How do I look after implants?
Cleaning access and maintenance matter. We’ll show you what to do and what tools help. Read: How to clean dental implants.
Are implants better than a bridge?
Often, yes — because you may avoid trimming healthy neighbouring teeth. But it depends on your bite, bone, and gum health.
Do you offer finance?
Yes — we can discuss options (up to 12-month finance) during your visit so you can plan comfortably.
What if I’m nervous?
That’s common. We go at your pace, explain first, and only proceed when you’re comfortable. You can also visit for a routine check-up first: Dental check-ups.
How do I book?
Book online, call, or message us — and we’ll guide you to the right option. No pressure — just clear advice and time to decide.

Ready to talk implants?
Call now, book online, or message us — we’ll guide you to the right option. No pressure — just clear advice and time to decide.
Address: 341 Birmingham Road, Great Barr, Birmingham, B43 7AP
